Learning objectives
|
Introduction
The overriding concept in hyperacute care is that "time is brain" and that systems must be in place to rapidly receive acute stroke patients and quickly assess them. There are two real streams, those who may be suitable for urgent therapies and the rest. Urgent therapies would include Stroke Thrombolysis and Mechanical Thrombectomy and reversal of anticoagulation for those with ICH on anticoagulants and those deteriorating due to massive stroke due to oedema or hydrocephalus or haematoma who may benefit from decompression, External ventricular drainage (EVD) or craniectomy. These patients will become immediately apparent.
Prehospital Stroke Care
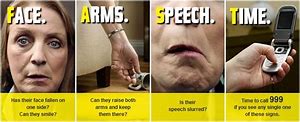
Prehospital stroke care is focused on acute care such as initial safety of the airway, breathing and circulation, blood glucose checking and then early recognition, identification and rapid access to specialist stroke care as quickly as possible. Some places have developed mobile stroke units where ambulances equipped with CT scanner, paramedics, nurse and stroke doctor attend the patient and give Alteplase (thrombolysis) en route. However there is no way to perform a thrombectomy. In the UK this happens in the UK at Southend and is seen in various centres in Europe and the USA and it is still regarded by many as a research topic with some sceptics. Most of the time the pathway is rapid assessment and using the FAST test to identify possible strokes which are brought to the nearest stroke centre. The latest reports suggest that the use of specialized stroke ambulances increases the proportion of patients receiving intravenous thrombolysis and shortens alarm-to-treatment time by approximately half an hour compared to standard care but direct effects of prehospital stroke care on functional outcome have yet to be shown
| Acute Pre Hospital Stroke Assessments |
|---|
|
Further reading on Prehospital care
Patients should be screened for hypoglycaemia with a capillary blood glucose, and for stroke or TIA using a validated tool.
NICE and RCP have published a Pre-hospital care concise guide for stroke 2016
- Those with sudden onset of focal neurological symptoms should be screened for hypoglycaemia with a capillary blood glucose, and for stroke or TIA using a validated tool.
- Those with persisting neurological symptoms who screen positive using a validated tool should be transferred to a hyperacute stroke unit as soon as possible.
- Suspected acute stroke (including inpatients) should be admitted directly to a HASU and be assessed for emergency stroke treatments by a specialist physician without delay.
- Ensure that people with conditions that mimic stroke are transferred without delay into a care pathway appropriate to their diagnosis.
- Ensure education programme for all staff providing acute stroke care (including ambulance services and the ED as appropriate)
- Ensure training for healthcare professionals in the speciality of stroke.
- Acute stroke services should participate in national and local audit, multi-centre research and quality improvement programmes.
- People who screen negative but in whom stroke is still suspected should be treated as if they have stroke until the diagnosis has been excluded by a specialist stroke clinician.
- The pre-hospital care of people with suspected stroke should minimise time from call to arrival at hospital and should include a hospital pre-alert to expedite specialist assessment and treatment.
- Patients with suspected stroke whose airway is considered at risk should be managed appropriately with suction, positioning, and airway adjuncts.
- Patients with residual neurological symptoms or signs should remain nil by mouth until screened for dysphagia by a specially trained healthcare professional.
- Patients with suspected TIA should be given 300mg of aspirin immediately and assessed urgently within 24 hours by a specialist physician in a neurovascular clinic or an acute stroke unit.
- Patients with suspected stroke or TIA should be monitored for atrial Fibrillation and other arrhythmias.
 |  |
| We must be constantly reviewing pathways to ensure maximum efficiency |